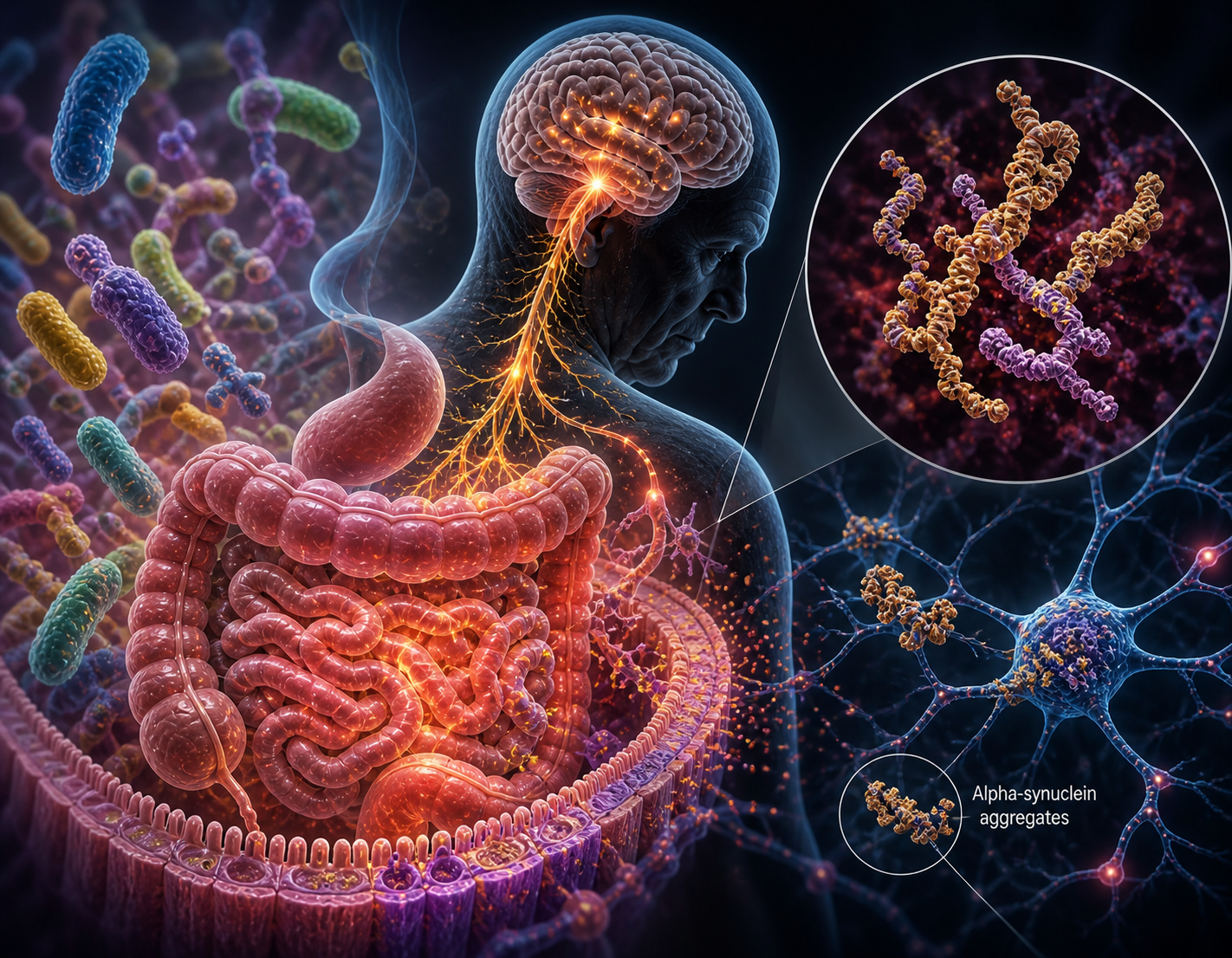
Parkinson’s disease is increasing at a rapidly growing rate worldwide. The number of diagnosed patients is rising in communities like never before. More people are developing the disease as they age and because doctors are identifying it more actively through improved diagnosis. The predicted numbers in multiple studies range from 1.2 million in the U.S. to 25.2 million worldwide by 2050. Those numbers will get higher as our population continues to age and the influence of pesticides and chemicals influence continues to change our bodies by damaging our nervous system though Neurotoxicity, disrupting hormonal balance and lead to impaired fertility in both men and women, birth defects, and developmental problems in children (National Institute of Environmental Health Sciences), and causing damage to DNA, increasing the risk of developing cancers such as non-Hodgkin Lymphoma, Leukemia, brain, prostate, and kidney cancers according to the National Library of Medicine.
How Does Telehealth/Telemedicine Benefit Parkinson’s Patients?
According to this 2023 study in Nature, an estimated 90% of people living with Parkinson’s disease in the U.S. were covered by Medicare health insurance in 2019, but an estimated 40% did not see a neurologist during the 2019 calendar year, and only about 9% received care from a movement disorder specialist. Demographics from the study indicate that people living with Parkinson’s were 2.3% Asian, 5.9% Black, 2.6% Hispanic, 0.3% North American Native, and 85.3% White. The study highlights that people of color are less represented among people with Parkinson’s on Medicare (14.7%) compared to the overall Medicare population (20.7%). This gap is even larger for black beneficiaries, who make up only 5.9% of those with Parkinson’s, compared to 10.5% of the total Medicare population. However, there is no data to specifically clarify whether this is due to delayed or underdiagnosis of Parkinson’s disease among people in areas with more income-restricted populations, or a lack of neurologists available in a given region. This is where Telehealth or Telemedicine could give patients and doctors an advantage.
There are many benefits and opportunities for people who don’t live near a neurologist, health care facility, or movement disorder specialist because of distance or who just have trouble traveling. Access to a specialist via an internet connection allows people to avoid transportation and healthcare issues from their own homes. This also allows for follow-up visits during weather delays and support for physical, speech, and occupational therapies. Using wearable sensors, smartphone apps, and remote testing for bradykinesia, tremor, and gait, many patients find telemedicine as effective as any home delivery service.
Telemedicine has many supporters in the medical community, including Dr. Michael Okun and Dr. Ray Dorsey, authors of the book Parkinson’s Plan. “Telemedicine is not just a convenience; it is the next frontier in Parkinson’s care. The future of this disease will depend on our ability to move expert, multidisciplinary care from the clinic into the home. When care travels to where folks live, we reach the underserved, reduce barriers, and create a continuous, connected model that truly centers on the person living with Parkinson’s,” according to Dr. Okun.

Like everything we create, not all of it withstands scrutiny. Setting up futuristic medical treatments has its challenges and pitfalls, with the most significant obstacle always seeming to be money. Not all regions or insurers reimburse tele-visits equally; cross-state licensing can complicate seeing specialists in other locations. What might be in-network for you could be out-of-network for someone else. Some states require private health insurers to cover telehealth visits, while others mandate reimbursement for telehealth at the same rate as in-person visits. Some states have no specific laws on the books at all.
“Virtual house calls for chronic diseases like Parkinson’s are not only as effective as in-person care, but broader adoption of this technology has the potential to expand access to patient-centered care, says Dr. Dorsey, but states, “Yes, expanding, but Medicare coverage is tenuous, and most with Parkinson’s disease receive suboptimal care to say the least.”
Incomplete physical examinations have limitations and drawbacks. Several key neurological assessments cannot be accurately performed during a virtual exam. Rigidity (resistance to passive limb movement) is a hallmark sign of Parkinson’s disease. It helps differentiate Parkinson’s from other movement disorders, such as Essential Tremor.
Rigidity can only be felt, not seen, and requires a healthcare provider to move the patient’s limbs to evaluate resistance through the range of motion. While patients can describe what they may be feeling, which can be subjective, a hands-on approach provides a more accurate diagnosis. Deep tendon reflexes at the knee, ankle, and biceps help a healthcare provider assess the condition of the spinal cord and also help identify neuropathy, upper motor neuron lesions, or early signs of myelopathy.
Other challenges facing Telemedicine include users’ ability to confidently use their own laptops or desktops and operate their webcams, making less tech-savvy people less likely to participate from home. As with any telehealth setup, data security, HIPAA compliance, and the safe handling of video or sensor data also matter.
A recent review in Nature found that interest in telemedicine declines as disease severity increases; only about 60% of advanced-stage patients are willing to use telemedicine, vs. 70% in early stages.

If you and your healthcare provider are considering telehealth for Parkinson’s disease, here are practical tips:
- Ensure good video quality by using adequate lighting and proper camera placement.
- Having a caregiver or assistant present is helpful for camera adjustments and overall safety.
- Prepare a list of symptoms, medication changes, and questions in advance.
- For motor exams, ensure there is enough space to walk and move the camera.
- Not every patient or visit is suitable for telehealth. Patients with severe motor fluctuations or frequent falls may need in-person supervision.
- Start with simple virtual visits and expand as comfort increases.
Many patients appreciate the personal, hands-on care a healthcare provider offers. Their offices are specially designed for patient care, so it might not feel the same to you, but it’s up to you and your healthcare provider to find what works best for your needs. For Parkinson’s patients, especially, finding a good balance between staying at home and visiting the doctor could benefit both you and your provider in the short term. As the disease progresses, it will be up to both of you to decide what’s best for ongoing care.
Media by Chris Denny/Adobe